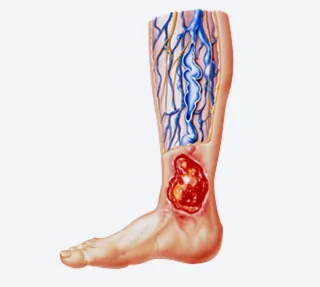
Preventing venous ulcers is all about keeping blood flowing smoothly in the legs — small daily habits can stop them before they start. Here's a simple breakdown by category:
Lifestyle Changes
Maintain a healthy weight: This is a crucial baseline and one that’s largely controllable. Extra kilos squeeze leg veins, thereby increasing risk. Indian carb-heavy, protein deficient diets do not help the matter. More balanced meals, eating patterns (eating protein before the carbs) and portion control go a long way.
Work out: Walk, swim, cycle or run 30 minutes daily to activate your calf muscles, which pump blood upward. Play a sport if ‘working out’ feels boring. Most sports involve some amount of calf work.
Quit smoking: It hardens arteries and worsens vein strain — seek patches, support groups and therapy.
Daily Leg Care
Leg Elevation: Raise the legs up to 15-30 minutes, about 3-4 times a day, especially after prolonged standing. Foot elevation pillows really help, as they make it more practically feasible on a bed or sofa.
Compression Stockings: If at risk (like varicose veins), compression stockings 20-30mm Hg can be worn during the day.
Vein Health Management
Control comorbidities: Keep blood pressure, diabetes, and cholesterol in check with meds and diet. For blood pressure, in particular, mindful practices like breath-work can help. Diabetes and cholesterol come down to dietary choices and environment design. For example; reduce the amount of sugar stocked at home. If an ingredient is in short supply, you tend to use less of it.
Early varicose vein treatment: Undergo early treatments like laser ablation or injections at the onset of varicosities (bulging signs) to avoid graduation into ulcers.
On a generalized note, moisturizing skin regularly and avoiding tight, non-breathable clothing helps too.