Minimally invasive approaches now allow for surgery with small thoracotomy incisions (6-7 cms) for direct access, and significantly lower infection risks.
Rapid-deployment valves: These ‘snap-in’ tissue valves use a balloon to expand, reducing surgery time and bleeding.
Ross Procedure: For younger patients, they swap the aortic valve with the pulmonary valve (plus a donor pulmonary), so there’s no need for blood thinners for life.
Hybrids: Like HCR (Hybrid Coronary Revascularization), which is a combination of minimally invasive CABG Surgery and angioplasty, surgical and catheter approaches are used for aortic conditions too. Surgical teams take these calls based on the coronary anatomy, and overall risk profile.
Benefits of AVR Surgery
Aortic Valve Replacement can transform life quality by addressing the root cause of multiple symptoms and protecting long-term heart health. AVR replaces a faulty valve with either a mechanical one (made of metal, lifelong durability but requires blood thinners) or tissue (from pigs or cows, no blood thinners needed but the durability is 10-15 years). Either of these restore smooth blood flow, halt the progression of heart failure, and significantly improve survival outcomes — many patients live 10-20+ years of active life after the surgery.
Some of the benefits include increased enthusiasm for walking and other physical work like gardening, or even spending time with family. Hemodynamics are greatly enhanced, making exercise, light sport and travel possible without constant dizziness or fatigue.
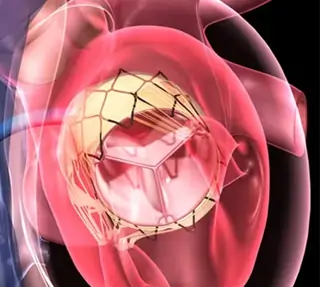
Of the different approaches, TAVR shines for quick wins: Just 1-3 days in the hospital as compared to 5-7 days for SAVR, with less pain and fatigue. Driving and work can resume in weeks, not months. SAVR patients often take 6-12 weeks to fully recover with rehab.